St. Louis—A comprehensive new study has revealed that GLP-1 receptor agonists, blockbuster drugs widely known for treating diabetes and obesity, may significantly lower the risk of addiction across multiple substances. The findings were published in a major medical journal on March 4, 2026. Researchers analyzed medical records from over 600,000 veterans in the U.S., uncovering dramatic reductions in both the development of new addictions and the occurrence of severe outcomes like overdoses among those already struggling with substance use.
Below is a detailed examination of how GLP-1 medications might fight addiction and reshape treatment approaches.
Context & Background
How did this research originate? Physicians initially noticed anecdotal evidence of patients losing interest in alcohol and nicotine after starting GLP-1 medications for weight loss or diabetes. Dr. Ziyad Al-Aly and his team at Washington University in St. Louis initiated a massive observational study using electronic health records from the U.S. Department of Veterans Affairs to test if these drugs curbed cravings across the board.
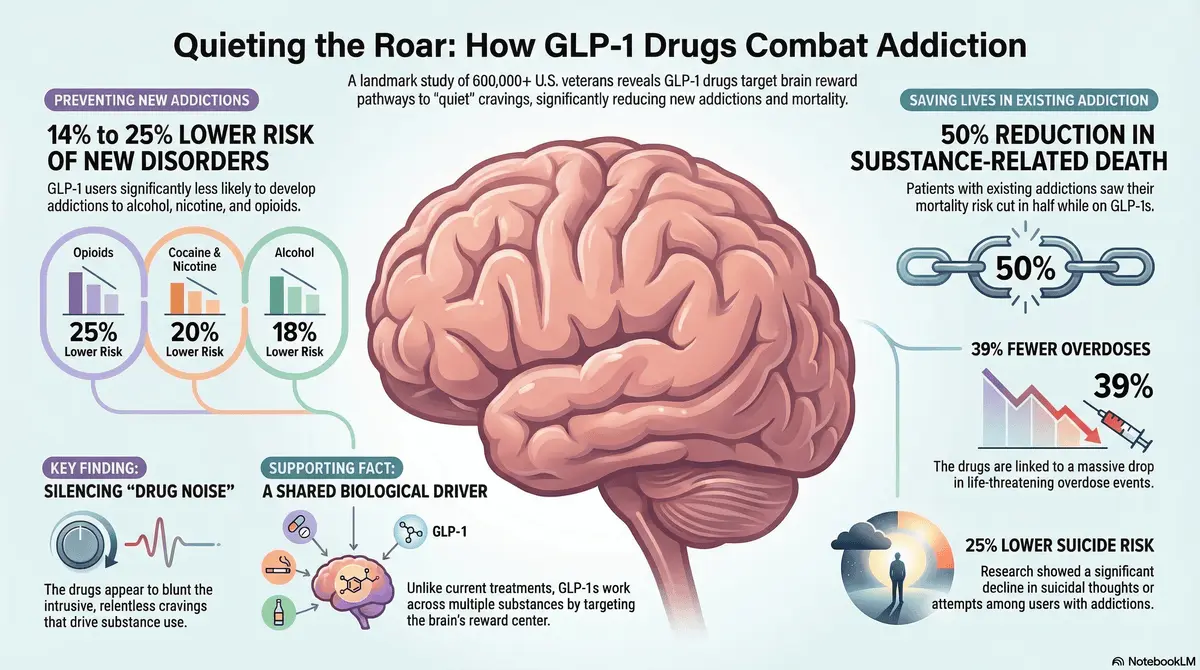
The key biological mechanisms Researchers believe that GLP-1 receptors are not only present in the gut but also highly concentrated in the brain’s reward and motivation pathways. Just as the drugs suppress the persistent, intrusive thoughts known as “food noise,” they appear to dampen “drug noise,” effectively silencing the underlying biological cravings that drive addiction.
Why this matters for public health Addiction is a leading cause of sickness and death globally, with existing treatments often limited to specific substances and yielding high relapse rates. Because GLP-1 drugs show efficacy against a broad spectrum of addictions—including cocaine, cannabis, and opioids—they could provide a unified pharmacological approach where few or no approved medications currently exist.
Q&A: Unpacking GLP-1 Treatments for Addiction
Q: WHY do GLP-1 medications seem to work across entirely different types of addictive substances?
A: These medications target a shared underlying biological vulnerability in the brain’s reward centers rather than the specific chemical pathways of individual drugs.
- Receptor Location: The GLP-1 hormone binds to receptors in brain regions governing motivation, reward, and impulse control.
- Craving Reduction: By dampening dopamine signaling in the brain’s core reward center, the drugs make addictive substances feel fundamentally less rewarding.
- Symptom Alleviation: Animal studies suggest that GLP-1 drugs might also ease withdrawal symptoms, diminishing both the drive to use substances and the physical pain of stopping.
Q: HOW significant were the reductions in harm for patients with existing substance use disorders?
A: The study demonstrated substantial decreases in severe medical events and mortality among patients taking GLP-1s compared to those on other diabetes medications.
- Mortality Decrease: There was a 50% lower risk of death related to substance use.
- Overdose Prevention: Patients experienced a 39% to 40% reduction in drug overdoses.
- Hospitalization Drop: The data showed a 25% to 26% lower risk of hospitalizations and a 30% to 31% reduction in emergency department visits.
Q: HOW did the drugs impact the development of new substance use disorders?
A: For patients without prior addiction history, GLP-1 medications significantly lowered the statistical risk of developing new dependencies across all major substance categories.
- Opioid Prevention: Users showed a 25% reduced risk of developing an opioid use disorder.
- Stimulant Avoidance: The risk of developing cocaine and nicotine dependence dropped by 20%.
- Alcohol and Cannabis Decline: Patients had an 18% lower risk of developing an alcohol use disorder and a 14% lower risk for cannabis use disorder.
Q: WHY are medical professionals cautious about prescribing GLP-1s specifically for addiction right now?
A: The current findings are based on an observational study, meaning randomized controlled clinical trials are required to prove direct causation and determine safe, specific protocols.
- Unanswered Variables: It remains unclear if cravings return upon stopping the medication, or if the brain eventually adapts and erodes the drug’s benefits over time. At this time, long-term relapse rates after discontinuing GLP-1 therapies remain unverified by official sources.
- Side Effects: These medications carry risks such as nausea, vomiting, and rarely, pancreatitis, which must be carefully weighed against their potential benefits.
- Population Limits: The observational study predominantly evaluated older, white male patients in the U.S. Department of Veterans Affairs system, requiring further research across broader demographics.
Q: HOW might these findings shift the overall treatment landscape for addiction?
A: The broad efficacy of GLP-1s could transition addiction treatment from targeting individual substances to addressing the fundamental biological drive of craving itself.
- Addressing Treatment Gaps: Currently, there are no approved pharmacological treatments available for addictions to stimulants like cocaine or methamphetamine.
- Primary Care Integration: Because primary care doctors already prescribe GLP-1 drugs for diabetes and obesity at scale, addiction treatment could become vastly more accessible compared to relying solely on limited specialists.
- Dual-Benefit Potential: Patients suffering from obesity or diabetes alongside an addiction could effectively treat both chronic conditions simultaneously with a single medication.
Editorial Note & Transparency
Verification Log:
- Medical Journal: Data published in The BMJ detailing the efficacy of GLP-1 receptor agonists.
- Institutional Research: Analysis and demographic data provided by Washington University in St. Louis and the U.S. Department of Veterans Affairs.
- News Reporting: Synthesis of clinical findings from medical experts, institutional directors, and addiction specialists.
Compliance:
- Privacy:This article respects user data under our Privacy Policy.
- Transparency: No sponsored content influenced this reporting.
Contact Us: For corrections or feedback, please email: news.desk@qnanews.com