Atlanta/New York — Medical professionals nationwide are raising alarms over the increasing incidence of colorectal cancer among younger demographics, a group traditionally considered low-risk. Clinical observations highlight a concerning upward trend heading into March 10, 2026, which marks a critical point in National Colorectal Cancer Awareness Month. Recent high-profile deaths in younger adults have brought this issue to the forefront, prompting gastroenterologists to aggressively advocate for proactive screening and lifestyle interventions.
Below is a detailed examination of the rising rates, diagnostic symptoms, and preventative strategies surrounding colorectal cancer.
Context & Background
What is driving the rise in early-onset cases? While the exact biological cause remains under active investigation, medical experts attribute the increase heavily to shifting lifestyle factors and modern diets. Physicians point to rising rates of obesity, sedentary lifestyles, and the heavy consumption of ultra-processed foods as primary contributors that disrupt gut health.
The historical shift in patient demographics For decades, colorectal cancer was predominantly viewed as an affliction of older adults, with screening traditionally beginning past the age of 50. However, recent data indicates that incidence rates in individuals under 50 have increased significantly, with nearly half of all new cases now occurring in adults under 65.
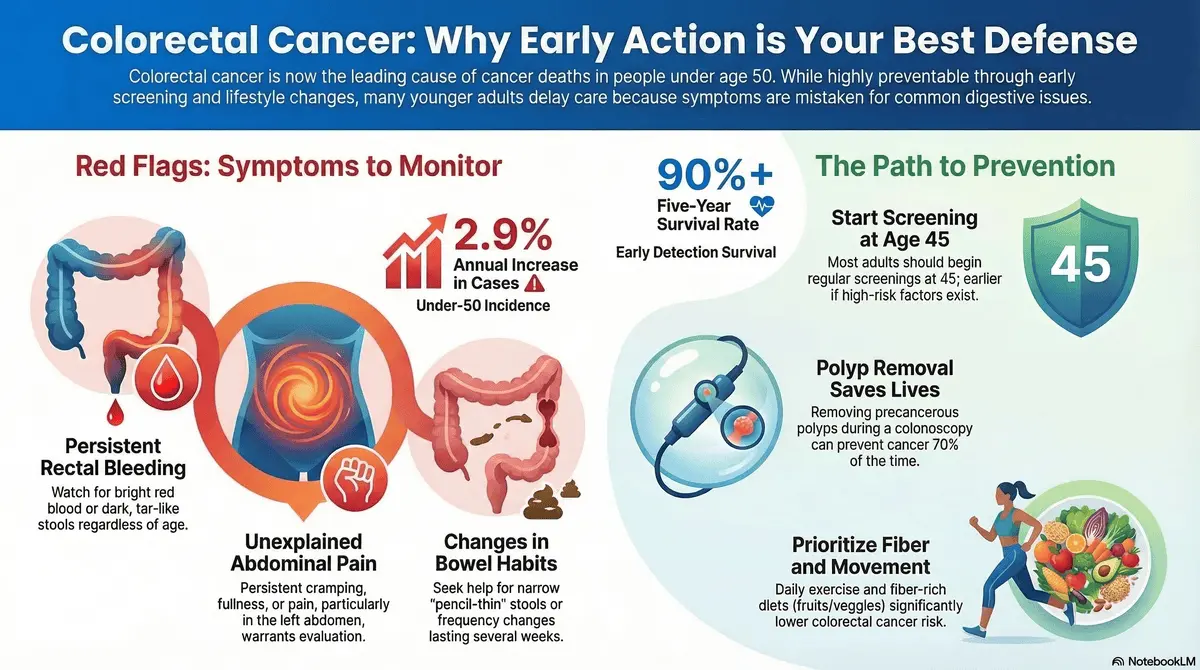
Why early detection matters Colorectal cancer often develops silently over several years without obvious early symptoms, but it is highly preventable when precancerous polyps are identified and removed. When captured early, the five-year survival rate for colorectal cancer is over 90%, underscoring the critical, life-saving nature of timely colonoscopy screenings.
The key players in clinical prevention Leading medical institutions and gastroenterologists, including Dr. Steve Georgopoulos of NYU Langone and Dr. Samir Gupta of UC San Diego Health, are actively reshaping public screening protocols. Organizations like the American Cancer Society now strongly recommend that average-risk adults begin routine screening at age 45 rather than waiting until age 50.
Q&A: Unpacking Colorectal Cancer Prevention and Diagnosis
Q: Why are doctors specifically monitoring everyday digestive habits to detect this cancer?
A: Routine digestive functions serve as the earliest, most direct indicators of cellular damage or physical blockages in the digestive tract.
- Blood Detection: Blood in the stool, whether bright red or dark, is a primary warning sign that is dangerously often mistaken for benign conditions like hemorrhoids.
- Bowel Changes: Persistent changes in bowel habits, including chronic constipation, diarrhea, or an unproductive urge to defecate, can indicate a tumor occupying space in the rectum.
- Pain Patterns: Unexplained, persistent abdominal pain, particularly on the left side, may signal a bulky mass limiting the normal passage of stool.
Q: How do lifestyle and dietary choices biologically impact the colon’s vulnerability to cancer?
A: Sedentary behavior and nutrient-poor diets alter the gut microbiome and drastically slow digestion, increasing the colon lining’s exposure to harmful substances.
- Microbiome Disruption: Diets high in processed foods and low in natural fiber disturb the balance of bacteria needed to produce vital anti-inflammatory compounds.
- Digestive Speed: Physical inactivity slows digestive motility, meaning potentially carcinogenic waste remains in contact with the colon lining for much longer durations.
- Nutritional Deficits: A lack of whole grains, fruits, and vegetables deprives the colon of essential nutrients that support a consistently healthy gut environment.
Q: How does a colonoscopy function as both a diagnostic and preventative medical tool?
A: Unlike many cancer screenings that only detect existing malignancies, a colonoscopy allows doctors to physically intervene before cancer can fully develop.
- Polyp Removal: Physicians can visually locate and immediately remove precancerous polyps during the procedure, stopping cancer before it begins.
- Visual Assessment: Utilizing a flexible tube with a digital camera, doctors thoroughly examine the entire colon, ensuring accurate and comprehensive evaluation.
- Technological Integration: Advanced facilities, such as Billings Clinic Bozeman, are now using FDA-cleared AI tools like the GI Genius module to highlight subtle areas that might otherwise go unnoticed by the human eye.
Q: Why might patients present with systemic symptoms like severe fatigue rather than localized digestive issues?
A: Tumors can cause insidious, hidden effects on the body’s overall resources before ever causing a direct physical blockage in the digestive tract.
- Hidden Bleeding: Slow, internal blood loss from a tumor at the start of the colon can lead to iron deficiency anemia, manifesting as severe fatigue, shortness of breath, and weakness.
- Nutrient Absorption: Cancer can impair the digestive system’s biological ability to properly absorb essential nutrients, leading to rapid, unintentional weight loss.
- Metabolic Drain: The presence of a malignancy often affects appetite and metabolic function, contributing to a sudden drop in body weight without conscious dietary changes.
Q: How are medical professionals addressing the rising incidence among younger, asymptomatic patients?
A: The medical community is rapidly shifting baseline guidelines and urging heightened clinical vigilance to catch the disease in demographics previously considered safe.
- Guideline Adjustments: The recommended age for average-risk screening has been officially lowered from 50 to 45 by major health organizations, including the Centers for Disease Control and Prevention.
- Symptom Evaluation: Doctors, including Dr. Derek Ebner at the Mayo Clinic, advise thoroughly investigating symptoms like rectal bleeding in younger patients rather than immediately assuming benign causes.
- Genetic Profiling: Patients with a family history or inherited conditions are being directed to specialized high-risk programs for earlier and significantly more frequent screening schedules.
Editorial Note & Transparency
Verification Log:
- Clinical Guidelines: Sourced from official statements by the American Cancer Society, the Centers for Disease Control and Prevention, and medical professionals at UC San Diego Health and the Mayo Clinic.
- Statistical Data: Incidence rate trends among adults under 50 verified through epidemiological reports cited by multiple oncologists and gastroenterologists.
- Symptom Profiles: Diagnostic criteria corroborated by clinical experts including Dr. Derek Ebner, Dr. Samir Gupta, and Dr. Steve Georgopoulos.
Compliance:
- Privacy: This article respects user data under our Privacy Policy.
- Transparency: No sponsored content influenced this reporting.
Contact Us: For corrections or feedback, please email: news.desk@qnanews.com