Washington/New York — Colorectal cancer has officially become the leading cause of cancer-related deaths among adults under the age of fifty in the United States. Following updated medical guidance publicized heavily on March 12, 2026, health professionals are urgently warning younger demographics to prioritize early screenings and remain vigilant about subtle symptoms. Driven by shifting dietary habits, sedentary lifestyles, and newly discovered tissue biomechanics, the disease is increasingly presenting at advanced, harder-to-treat stages in younger populations.
Below is a detailed examination of the early-onset colorectal cancer epidemic and the preventative strategies currently advised by the medical community.
Context & Background
What is driving the increase in early-onset cases? Experts point to a complex combination of sedentary lifestyles, obesity, and diets high in ultra-processed foods and red meat as primary catalysts. Researchers also suspect a birth cohort effect, suggesting generations born after the 1950s have been exposed to progressive environmental risks, with microplastics emerging as a highly suspected, though unproven, factor.
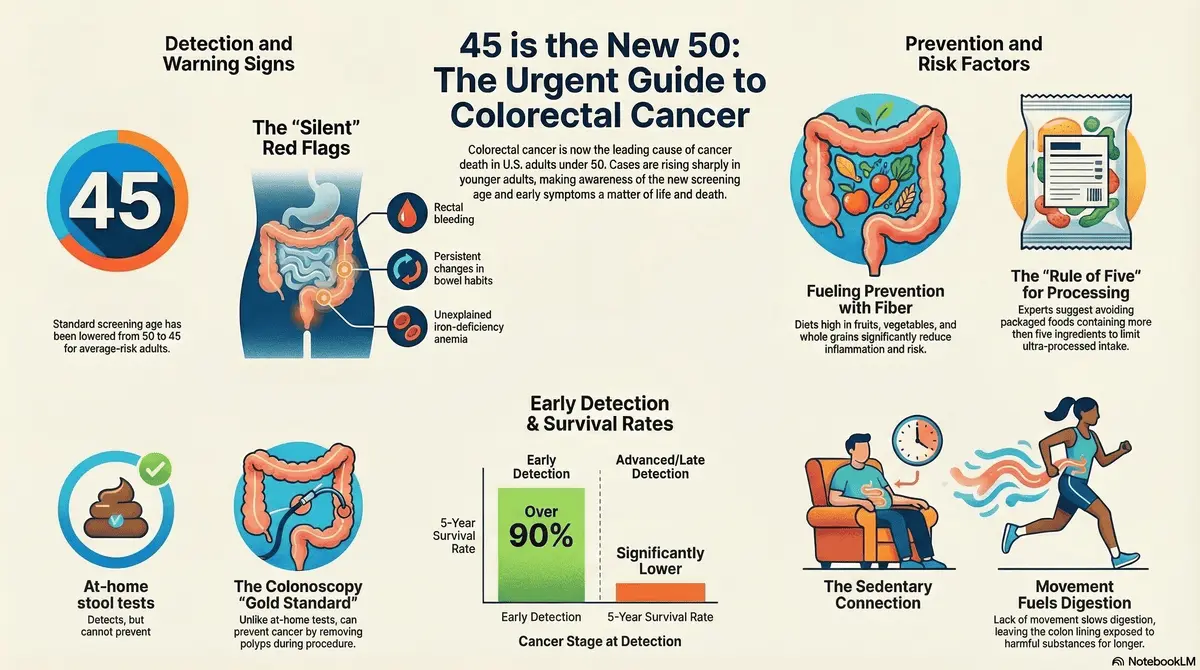
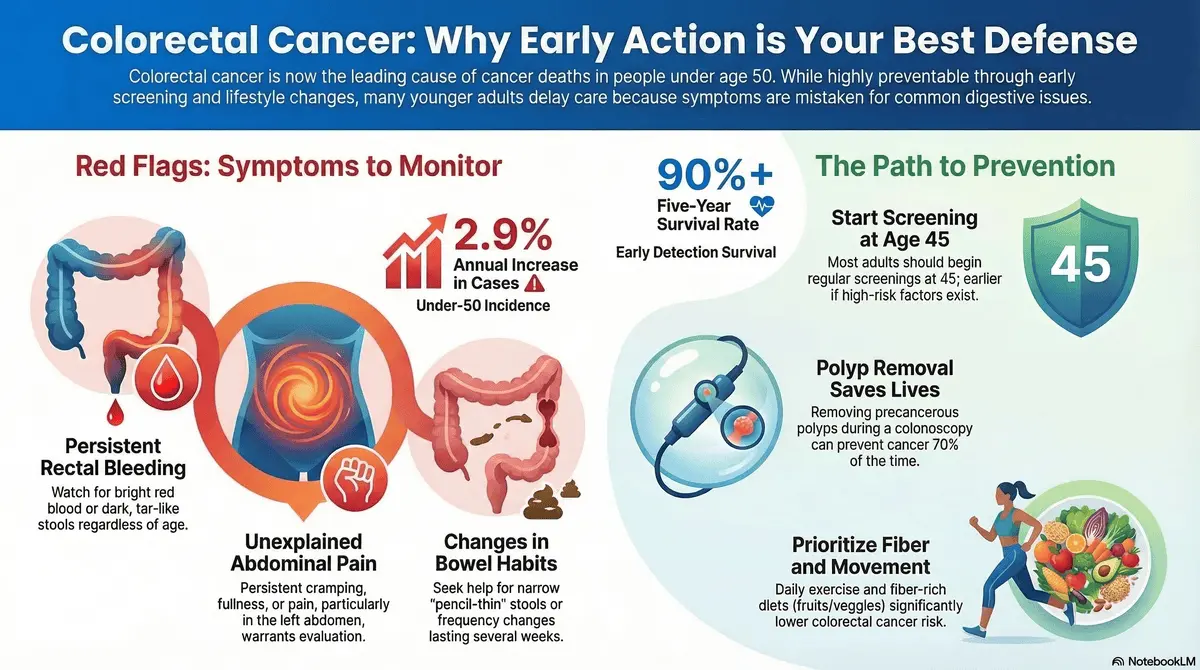
How have medical guidelines adapted? In response to the sharp demographic shift in diagnoses, national health organizations have lowered the recommended age for initial colorectal cancer screening from fifty to forty-five for average-risk individuals. Preventive diagnostic tools, specifically colonoscopies, allow doctors to safely identify and extract precancerous polyps years before they can develop into malignant tumors.
Who are the key medical voices sounding the alarm? Leading epidemiologists such as Rebecca Siegel of the American Cancer Society, alongside gastroenterologists like Dr. Derek Ebner at the Mayo Clinic, are actively working to dispel the outdated myth that colon cancer is strictly an elderly disease. They emphasize that younger patients habitually dismiss critical warning signs like rectal bleeding, assuming they are minor issues, which critically delays life-saving interventions.
Q&A: Unpacking Early-Onset Colorectal Cancer
Q: Why is early-onset colorectal cancer frequently diagnosed at highly advanced stages?
A: Younger patients consistently overlook severe gastrointestinal symptoms and delay preventative screenings due to deeply ingrained misconceptions about their age-related risk levels.
- Symptom Dismissal: Individuals routinely attribute warning signs, such as bright red blood in the stool, to benign conditions like hemorrhoids, avoiding professional medical evaluation.
- Screening Protocols: Because standard preventative colonoscopies are generally not recommended or covered by insurance until age forty-five, younger patients rarely receive asymptomatic imaging.
- Diagnostic Hesitancy: At this time, the exact reason why some primary care providers may overlook cancer symptoms in young adults remains unverified by official sources, though specialists note doctors are traditionally accustomed to treating the disease almost exclusively in elderly populations.
Q: How do newly discovered biomechanical factors influence tumor growth in younger patients?
A: Bioengineering studies reveal that early-onset colorectal cancer patients possess abnormally stiff colon tissue that actively promotes aggressive tumor development.
- Tissue Rigidity: Researchers discovered that both cancerous and surrounding noncancerous colon tissues in younger patients are mechanically stiffer compared to tissues from older colorectal cancer patients.
- Collagen Accumulation: The extracellular matrix within the colon wall of younger patients exhibits fibrotic characteristics, containing excessive amounts of collagen that rigidify the tissue structure.
- Accelerated Multiplication: When cancer cells are placed in these artificially stiff, scar-like environments during laboratory testing, they multiply at a significantly faster rate.
Q: How does modern nutritional intake specifically impact the gut microbiome and cancer risk?
A: Diets deficient in natural fiber and high in chemical additives disrupt the delicate bacterial balance in the colon, fostering chronic tissue inflammation.
- Fiber Deficiency: A lack of whole grains, legumes, and vegetables reduces the production of short-chain fatty acids like butyrate, which are necessary to fight inflammation and support colon cell health.
- Chemical Additives: Ultra-processed foods, which are high in lipids, salt, and preservatives, act as nutrient-poor calories that increase obesity rates—a well-documented cancer risk factor.
- Bacterial Imbalance: Without a healthy microbiome, the colon lining is exposed to potentially harmful compounds, toxins, and bile acids for longer durations, which accelerates cellular damage over time.
Q: Why is a sedentary lifestyle considered a direct mechanical threat to colon health?
A: Chronic physical inactivity drastically slows down digestive motility, increasing the total time toxins remain in direct contact with the vulnerable colon lining.
- Sluggish Digestion: Extended periods of sitting reduce intestinal stimulation, causing waste and potential carcinogens to linger in the digestive tract rather than passing efficiently.
- Insulin Disruption: A lack of daily exercise negatively affects insulin sensitivity and regulation, which can foster a biological environment highly conducive to cellular mutations.
- Inflammatory Response: Sedentary habits contribute to chronic, low-grade inflammation throughout the body, further compromising the immune system’s ability to clear abnormal, precancerous cells.
Q: How are genetic syndromes and family histories altering preventative screening timelines?
A: Individuals with specific hereditary conditions or familial histories of the disease are now urged to begin preventative screenings decades before the standard age of forty-five.
- Familial Proximity: Patients with a first-degree relative diagnosed with colon cancer are advised to begin screening at age forty, or ten years prior to their relative’s initial diagnosis age.
- Lynch Syndrome: Those carrying this specific inherited DNA mutation face a drastically increased lifetime risk and must undergo colonoscopies as early as twenty to twenty-five years old.
- Polyposis Conditions: Patients diagnosed with Familial Adenomatous Polyposis carry a nearly guaranteed lifetime risk of colorectal cancer and are heavily recommended to start annual screenings between ten and twelve years old.
Editorial Note & Transparency
Verification Log:
- Medical Organization: Guidelines sourced from the American Cancer Society and National Cancer Institute regarding screening ages and mortality rates.
- News Outlet: Reporting compiled from The Guardian, Fox News, and TODAY covering patient testimonials and demographic shifts.
- Research Institution: Biomechanical findings regarding colon tissue stiffness sourced from the University of Texas at Dallas and UT Southwestern Medical Center.
Compliance:
- Privacy: This article respects user data under our Privacy Policy.
- Transparency: No sponsored content influenced this reporting.
Contact Us: For corrections or feedback, please email: news.desk@qnanews.com